Dr. Mauk’s Boomer Blog
Each week, Dr. Kristen Mauk shares thoughts relevant to Baby Boomers that are aimed to educate and amuse.
Dr. Kristen L. Mauk, PhD, DNP, RN, CRRN, GCNS-BC, GNP-BC, FAAN

Five tips for Grandparents to stay connected with family
With the birth of my daughter’s second child, I began to reflect on the important role that grandparents can play in the lives of their grandchildren. Here are five essential tips for older adults who want to have a lasting influence in the lives of their children and grandchildren.
Visit often. For those of us fortunate enough to live near our children and grandchildren, it is easy to see them often. Grandparents may even be the caregivers while parents are working. Visits don’t always have to be planned. Sometimes the best family time is a spontaneous invitation to dinner and a movie. However, sometimes distance can prevent regular visits. Some grandparents make it a goal to see their distant grandchildren once every 6 weeks or every few months. Be sure to take advantage of technology for your time together. Set a regular time to Skype or do Face-time. Don’t miss out on the subtle changes in those early years while babies are growing. Exchanging pictures may help, but they don’t replace the in-person experience. You may even think of relocating to be closer to family. For older grandchildren, be sure to have their cellphone number. Text them often and exchange pictures to stay involved in their lives and let them know you are available to them. Even small connections throughout the week (but without being annoying to teenagers of course) can make a difference in your relationship with your grandchildren.
Offer to help in practical ways. Working parents with young children will need a break at times. Ask how you can best help. Offer to keep the children for an overnight while mom and dad have a special dinner or weekend getaway. Many grandparents like to take their grandchildren on trips without the parents. Places like amusement parks, the zoo, or day trips to the water park or national forest all provide good diversion and quality time with Grandma and Grandpa while giving parents a rest. For even more quality time, take the older grandchildren on a cruise, camping in the mountains, or to a resort without their parents. For the mom with a newborn, take meals to the house (if you live close), do her grocery shopping or laundry, or send her a new bathrobe to show you are thinking of her. A favorite role model of mine sends the grandchildren a “baby shower in a box” with all sorts of goodies when she can’t be present due to distance or health concerns.
Plan special activities. Special activities need not be expensive. This could mean a trip to the park with Grandma or a special morning walk each week with Grandpa. My father used to take every grandson on a bow-hunting trip when they turned 12 years old. This was a rite of passage for every boy in the family. Grandpa would mount their first deer head for them and buy them a special hunting knife to commemorate the occasion. The girls in the family would take a trip to a Disney resort while the men were hunting. Grandchildren remember these events forever.
Attend special events. How fortunate are the kids whose grandparents are able to attend basketball and volleyball games, swimming tournaments, and Grandparent’s Day at school! Take advantage of being able to attend those dance recitals and school plays. If you live far, plan your visits to be able to attend some significant events like graduations, wedding showers, or school performances. This makes lasting memories with your family.
Be a constant in their lives. My parents divorced when I was 9 years old, and my paternal grandparents were the one constant in my life at that time. When a child’s world is jolted by change, grandparents can be that steadying influence that doesn’t change. They provide stability and security in an unsteady world for a child. The most important thing to remember is to be there. You don’t have to be the all-star parent or grandparent, but your children will remember that you were there for them when it counted the most.
Guest Blog: Adjusting to Life After a Stroke
In America, stroke is the third leading cause of death. The brain and heart rely on each other to sustain basic functionality of the human body. The brain controls a large portion of the body’s range of capabilities and nerve signaling. Your brain has multiple purposes, but a single stroke can put those critical functions at risk. Communication, memory, emotional activity, and physical capabilities can all be affected when the brain is not operating at its utmost potential.
Difference Between a Stroke and a Heart Attack
A stroke and a heart attack may seem similar but are very different. Both ailments occur due to a shortage of oxygenated blood and blood flow, except strokes primarily affect the brain while heart attacks mainly target the heart. When the body’s blood flow to the heart is blocked, sometimes due to a blood clot, it can cause a heart attack. A stroke, on the other hand, can cause possible brain tissue to decay and long-term disability or death.
Stroke Causes
The leading cause of strokes is anything that leads to blocked blood supply or a burst blood vessel, cutting off the oxygen flow to the brain. A number of risk factors for a stroke, such as high cholesterol and obesity, can be medically managed or treated. Nevertheless, as with certain terminal conditions, particular risk factors are more challenging to address.
An individual’s lifestyle has a considerable effect on their health. Harmful choices can lead to chronic illnesses with detrimental long-term consequences. Nearly everything that goes into the body has the potential to affect your physical and emotional well-being. For example, eating highly processed fast food can possibly make the person feel groggy and lethargic, while a plant-based diet can help support a healthy immune system.
Controllable risk factors for a stroke are:
- Diabetes
- Lack of exercise
- High blood pressure
- High cholesterol
- Excessive alcohol or drug use
- Smoking
Uncontrollable risk factors include:
- Age: The risk of having a stroke doubles every ten years after the age of fifty-five.
- Race: Black and nonwhite Hispanic Americans are affected more than white Americans.
- Gender: Although strokes occur more regularly in men, women are more prone to suffer one later in life, placing them at higher danger of nonrecovery.
- Family history: Strokes are more likely to occur within families that carry genetic disorders.
Even if someone is taking good care of their body and do not carry any genetic risk factors, they can still be at risk due to:
- Geography: Strokes happen more in southeastern America than in the rest of the country, perhaps due to elements of the regional culture such as diet.
- Climate: Extreme temperatures increase the risk of a stroke.
- Economic and social circumstances: Particular evidence suggests that stroke cases are more prevalent in low-income communities.
Stroke Treatment
To properly treat a stroke, doctors must first determine the causes of the symptoms through a CT scan or other stroke tests. Stroke tests vary from simple physical analysis and blood analysis to more involved procedures such as echocardiograms, cerebral angiograms, MRI scans, or carotid ultrasounds. About a quarter of stroke survivors will suffer a second stroke, making immediate treatment vital.
Some steps to help stroke patients recover include seeking support and therapy, monitoring medications, being on the lookout for dizziness or imbalance, ensuring a healthy diet, and keeping the brain active. It is crucial to remember that recovering from a traumatic brain injury such as a stroke takes time and patience.
Recovery can be a long-term process. Hence, it is imperative to understand how the body and brain are affected. Refer to the following infographic made by Family Home Health Services for further information on brain recovery as well as stroke-prevention practices to incorporate into everyday life.
Glaucoma Symptoms
Background
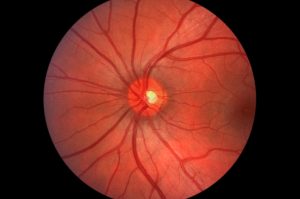
Glaucoma is a group of degenerative eye diseases with various causes that leads to progressive optic neuropathy, in which the optic nerve is damaged by high intraocular pressure (IOP), resulting in blindness. Glaucoma is a leading cause of visual impairment and the second leading cause of blindness in the United States; it occurs more often in those over 40, with an increased incidence with age (3% to 4% in those over age 70) (Fingeret, 2010; Kennedy-Malone et al., 2000; Podolsky, 1998).
Risk factors
Unlike cataracts, there are some ethnic distinctions with the development of glaucoma. African Americans tend to develop it earlier than Caucasians, and females more often than males. Glaucoma is more common in African Americans, adults over age 60 (especially Mexican Americans), and people with a family history (NIH, 2013). Other contributing factors include eye trauma, small cornea, small anterior chamber, cataracts, and some medications.
Signs and symptoms
Although the cause is unknown, glaucoma results from blockage that limits the flow of aqueous humor, causing a rise in intraocular pressure (IOP). Two major types are noted here: acute and chronic. Acute glaucoma is also called closed angle or narrow angle. Signs and symptoms include severe eye pain in one eye, blurred vision, seeing colored halos around lights, red eye, headache, nausea, and vomiting.
Symptoms may be associated with emotional stress. Acute glaucoma is a medical emergency and persons should seek emergency help immediately. Blindness can occur from prolonged narrow angle glaucoma.
Chronic glaucoma, also called open angle or primary open angle, is more common than acute (90% of cases are this type), affecting over 2 million people in the United States. One million people probably have glaucoma and don’t know it, and 10 million people have above normal intraocular pressure that may lead to glaucoma if not treated (University of Washington, Department of Ophthalmology, 2008). This type of glaucoma occurs gradually. Peripheral vision is slowly impaired. Signs and symptoms include tired eyes, headaches, misty vision, seeing halos around lights, and worse symptoms in the morning. Glaucoma often involves only one eye, but may occur in both.
Treatment
Since there is no scientific evidence of preventative strategies, early detection in those at risk is important. Treatment is essential to prevent loss of vision, because once vision has been lost to glaucoma, it cannot be restored. Diagnosis is made using a tonometer to measure IOP. Normal IOP is 10–21 mm Hg. Ophthalmologic examination will reveal changes in the color and contour of the optic nerve when glaucoma is present. Gonioscopy (direct exam), which is performed by an optometrist or ophthalmologist, provides another means of evaluation. Older persons and those at higher risk should have a yearly eye exam to screen for glaucoma.
Treatment is aimed at reducing IOP. Medications to decrease pressure may be given, and surgical iridectomy to lower the IOP may prevent future episodes of acute glaucoma. In chronic glaucoma, there is no cure, so treatment is aimed at managing IOP through medication and eye drops. Consistent use of and correct administration of eye drops is important. Older adults should be assessed for safety related to visual changes and also reminded to schedule and attend regular visits with their ophthalmologist.
Adapted from Mauk, K. L., Hanson, P., & Hain, D. (2014). Review of the management of common illnesses, diseases, or health conditions. In K. L.
Mauk’s (Ed.) Gerontological Nursing: Competencies for Care. Sudbury, MA: Jones and Bartlett Publishers. Used with permission.
Glaucoma Symptoms
http://www.nlm.nih.gov/medlineplus/tutorials/glaucoma/htm/index.htm
Guest Blog: Important Bathing Tips for Seniors
Important Bathing Tips for Seniors Searching for quick tips and ideas to make bathing safer for you or a loved one? Don’t miss this essential guide!
Fall-Proof the Bath/Shower
With seniors much more at risk for falling than non-seniors, it is critical to fall-proof one of the most hazardous rooms in the house – the bathroom. Install grab bars on the inside and outside walls of showers and tubs with wide grip surfaces to make holding and supporting yourself easier. Put down a non-skid mat outside of the tub or shower, as well as non-slip adhesive strips or mats that stick to the bottom of the bathing area.
Hang Toiletries
Simplify the entire process of shampooing and conditioning hair and lathering up with soap by hanging a toiletry dispenser over the shower head. Toiletry dispensers let you fill canisters with the liquids you use for bathing and access them hands-free in the shower (or often with the touch of a button). No more handling slippery bottles or bars of soap; toiletry dispensers are functional and safe and can be found online or in big box stores.
Wash Smarter
Good hygiene is paramount to your overall health and self-confidence and is just as important when you are a senior. If your old washcloth just isn’t cutting it anymore, invest in a low-cost bath scrubber that makes showering easier and more thorough. Hitting hard to reach places when you shower like your back and feet may be easier with a long-handled bath scrubber or loofah, preventing you from having to twist or bend over in a confined space like the shower.
Use a Removable Shower Head
As seniors age, agility and coordination may be compromised by weaker muscles and stiff joints. Instead of doing a dance in the shower to make sure you are fully rinsed off, get an easy-to-install removable shower head that allows you to better control the water flow and spray intensity. Handheld shower heads are also a smart addition to your bath or shower if you sit on a shower chair to bathe.
Being able to shower or bathe oneself plays an important role in maintaining independence and even being able to live on one’s own without assistance. For aging adults, taking precautions early with safety equipment and smart yet simple upgrades like toiletry dispensers may help prevent falls or injuries down the line.
Guest Blog: What You Need to Know About a Hemilaminectomy Procedure
This procedure is one of the safest, most minimally invasive treatments for a herniated disc. A Hemilaminectomy procedure is performed on patients with lumbar spinal stenosis. This diagnosis can come from several issues, such as Arthritis in the spine, which all result in pinched nerves. This procedure is perfect for someone suffering from a condition that occurs when the nerves are being pinched, resulting in severe pain running down the legs and into the feet. So here is what you need to know about the Hemilaminectomy procedure.
What is a Hemilaminectomy Procedure?
A hemilaminectomy is a surgical procedure performed on patients afflicted with lumbar spinal stenosis. This type of spine disorder occurs when the spinal column disc has been compressed over time and onward, which causes ongoing severe pain and discomfort for the patient.
The lumbar spinal discs are cushions of cartilage that sit between vertebrae. This condition occurs because of the pressure that builds up on these discs over time, which causes the pain to be extreme.
How is the Hemilaminectomy Procedure Performed?
This surgery is performed through a small incision on the back. Then special retractors are used to push apart the muscles in the mid-section of the back. This is a much more delicate surgery that must be performed through a small incision.
Because of this, it is usually performed on anyone under general or spinal anesthesia. As long as there are no problems with the patient, they should be able to wake up from the surgery in a few hours and go home after a day or two. This procedure is the least invasive option for patients who have chronic problems with their back.
When You Should Consider a Hemilaminectomy Procedure
This operation should be performed when symptoms of chronic pain are present. Some of these issues can occur from a pinched nerve that travels from the back down to the legs. It is also a procedure that is an option when there is a pressing issue with any of the pinched nerve issues.
Sometimes, this spinal disc can become herniated, which means that the pressure has become too much for it to handle and causes pressure on nearby nerves or bones. This is one of the most common conditions seen in lumbar spinal stenosis.
Sometimes, you can freeze off this spinal disc with a surgical fix by freezing it with an instrument, but Hemilaminectomy is the ultimate fix for this condition.
How Long Does Recovering Take After the Procedure?
Patients who undergo the Hemilaminectomy procedure will benefit immediately from this operation. After the surgery, most people have a day of recovery time before they are allowed to go home.
In most cases, patients return and participate in their normal activities within a few weeks of their Hemilaminectomy surgery. This general timeline is important because it provides comfort to the patient, knowing what they should expect when they decide to undergo this type of surgery.
The Risks of a Hemilaminectomy Procedure
As with any surgery, some risks come with it. Risks can include internal and external problems that may arise during the procedure. Some of these risks can include:
- Blood clots in the legs
- Bleeding
- Nerve damage
- Infection
- Spinal Fluid Leakage
- Allergic reaction to the anesthesia
In addition to this list, some risks are more common after a Hemilaminectomy procedure. This is because it is a less invasive surgery involving limited incisions in the patient’s back. After several months into the recovery process, it is possible at some point for the herniated disc to be recurring to a small degree.
This is something that most patients don’t have to worry about after a few months of recovery, but some patients do deal with a recurrent disc for the rest of their life. In such cases, it is important to get checked regularly.
Conclusion
The Hemilaminectomy procedure has become the preferred choice for most doctors regarding a full spine fix. This is because this procedure involves less invasive incisions, resulting in quicker recovery and improved patient comfort. This type of surgery is an option that is best for patients with debilitating conditions that affect their daily lives.
Five Tips to Surviving Your Husband’s Retirement
I remember when my father retired at the age of 62 from a busy career as a pediatric surgeon. I thought he would be bored, but he had already compiled a notebook full of chores to do around the house, places he wanted to go, and a bucket list of other accomplishments that had been put on hold. Shortly after his retirement, my Mom confided in me that it was a bit of an adjustment having Dad home all the time. Suddenly, Mom said she seemed to no longer be able to cook right after about 40 years of doing this on her own. Dad had a better way to do things, after all. Once I saw Mom trying to wrap a gift and the wrapping paper seemed too small for the size of present. Dad was trying to give her step by step instructions and after snapping at her, Mom let him wrap the gift himself. Now, while I do concede that Dad was able to wrap the gift absolutely perfectly with the allotted paper, Mom and I gave each other a knowing glance and smiled. Ah, retirement.
So, when my own husband announced that he was going to retire and sell his share of the business at the age of 51, I knew I had to take some action to give our marriage the best chance to survive and thrive against this new challenge. After all, when my father-in-law retired, my mother-in-law had to encourage him to get a part-time job so she could have some “peace”. Even she was a bit concerned when my husband decided to take early retirement. Here I offer my short bit of wisdom, gleaned not only from my own experience but also from many wise women who gave me their sage advice to prepare for this season of life: when your husband retires.
Set the ground rules. I had fortunately learned during a brief period when my husband was working from home that there were certain things that would have to be agreed upon before he ever retired if we were to live peaceably. For example, he was not allowed to take over any of my former responsibilities unless I asked him to. Driving the kids around to activities can be helpful, but trying to wash the shrinkable clothes was not. Taking us out to eat after I worked all day was fine, but trying to take over the kitchen was off limits. Helping the kids with business math (not my area of expertise) was great, but trying to be the full-time homeschool Dad was not going to work for any of us.
Have separate work spaces. Jim and I cannot share a computer. I teach partially online and spend lots of time working from home with consulting. We agreed early on that he would set up a separate place in a different part of the house for his computer and desk. This has created much harmony over sharing the work space.
Allow everyone time to adjust to the change. I must admit that it took me several weeks, maybe even months, to realize that my husband was truly going to retire. Once he was home all the time, the reality gradually set in, but I kept reminding myself to give us all an adaptation period as if we were starting a new job orientation, because things were definitely going to change. Our two teenagers were the most leery of Dad being home all the time. For them, the ground rules (i.e. “please just let us do our work and don’t change our routine”) were particularly essential.
Accept your differences. My husband is a problem-solver and savior. He likes a challenge and wants to fix everything for everyone if he can. While I admire this about him, I didn’t want him to fix the nice structure and functionality by which our home was already running. I learned to embrace his strengths and encourage him to accept my weaknesses (like overindulging in carbs and worrying about things I can’t control). He likes to exercise every day, watch sports, and spend time on the landscaping. I would rather take the kids to the movies and go shopping. And that had to be ok.
Embrace the positives. While I was a bit skeptical about how our lives would change with my husband retiring so soon, there are so many things to celebrate that I am daily embracing the wonderful opportunities and blessings that his retirement has brought to our family. We are free to travel more. He accompanies me on business trips, even to China twice! He is much more relaxed and pleasant. It makes our family happy to see him have the time and resources to do what he enjoys. Jim keeps busy all of the time and yet does not have the daily pressure of work-related stress. We spend more time with family and have plans to move nearer to the grandchildren and to a better climate.
For all the women who are warily facing their husband’s retirement, take heart. I can honestly say that with some forward and deliberate planning, my husband’s retirement is one of the best things that has ever happened to us!